Modern interventional cardiology in Montreal makes it possible to treat complex heart conditions and be home in less than 24 hours, without the trauma of open-chest surgery.
- This is achieved through minimally invasive techniques like TAVI and advanced stenting, which require only small punctures instead of large incisions.
- Success depends on your active role, from mental prep and asking the right questions to navigating the Quebec healthcare system effectively.
Recommendation: Understand your options and how to partner with your medical team for the best and fastest recovery possible.
The thought of heart surgery can be overwhelming. For many, it brings to mind images of long hospital stays, significant pain, and a difficult, months-long recovery. This fear is a major source of anxiety for patients and their families. While traditional open-heart surgery remains a vital tool, the landscape of cardiac care has been revolutionized. The focus has shifted dramatically towards minimally invasive techniques that are less about enduring a major operation and more about undergoing a precise, targeted intervention.
What if the key to a successful, rapid recovery wasn’t just in the surgeon’s hands or the advanced technology they use? What if it was also rooted in your own preparation and your active partnership with the medical team? This guide is designed from a nurse’s perspective to demystify advanced interventional cardiology as it’s practiced right here in Montreal. We’ll move beyond the generic advice and focus on what you truly need to know: how these procedures work, what to realistically expect during recovery, and how to navigate the local Quebec healthcare system to ensure you feel confident and in control every step of the way. Your journey to a healthier heart can be quicker and less daunting than you imagine.
This article will walk you through the key aspects of modern cardiac care in Montreal, from understanding the procedures themselves to planning your life after. We will explore the nuances of recovery, compare different treatment paths, and give you the tools to become an active participant in your own care.
Summary: Your Guide to Rapid-Recovery Heart Procedures in Montreal
- Angioplasty Recovery: Why Do Some Patients Feel Worse Before Feeling Better?
- TAVI vs Open Heart Surgery: Which Is Safer for Patients Over 75?
- How to Prep for a Cardiac Catheterization to Minimize Anxiety and Complications?
- The Subtle Chest Pain You Ignore That Signals a Blocked Artery
- How to Restart Physical Activity After a Stent Without Fear of Relapse?
- Public Hospital vs Private Clinic: Which Path Suits Your Urgency?
- How the Surgeon Controls the Robot: It’s Not Autonomous!
- Why Electrophysiology Is the Only Way to Permanently Cure Certain Arrhythmias?
Angioplasty Recovery: Why Do Some Patients Feel Worse Before Feeling Better?
It can be disconcerting. You’ve just had a successful angioplasty to open a blocked artery, and yet, in the first day or two, you might feel more tired or have some mild chest discomfort. This is a common experience known as the “recovery paradox.” Your body is healing from the intervention. The area where the catheter was inserted (usually the wrist or groin) needs time to recover, and your heart is adjusting to improved blood flow. While advanced protocols aim for a discharge in under 24 hours, it’s normal that most PCI patients are kept overnight for monitoring to ensure everything is stable before they head home. This initial phase of feeling “off” is typically temporary and a sign that your body has begun the healing process.
In Montreal, leading centers are actively working to make this process smoother and faster. The Montreal Heart Institute’s ERACS (Enhanced Recovery After Cardiac Surgery) program is a prime example. This protocol optimizes every step of the patient journey, from pre-admission to post-discharge care, to improve the patient experience and enable quicker, safer returns home. The focus is on managing discomfort proactively, encouraging early mobility, and providing clear instructions so you feel confident leaving the hospital.
Understanding this initial phase is crucial for your peace of mind. Instead of worrying, you can see it as the first step in a positive journey. The fatigue soon gives way to increased energy as your heart benefits from the restored circulation. The key is to listen to your body, follow the activity guidelines, and not push yourself too hard in the first 48 hours.
Your Post-Angioplasty Self-Audit Checklist
- Activity Check: Have I avoided all strenuous activities and heavy lifting for the first 48-72 hours as instructed?
- Mobility Goal: Am I engaging in light, short walks around my home to promote circulation without causing strain?
- Site Inspection: Am I checking the catheter insertion site (wrist or groin) daily for any signs of swelling, bleeding, or infection?
- Energy Log: Am I noticing a gradual increase in my energy levels day by day, even if it starts slowly?
- Follow-up Confirmed: Have I confirmed my follow-up appointment, typically required within 24-48 hours as per Quebec protocol, to review my progress?
TAVI vs Open Heart Surgery: Which Is Safer for Patients Over 75?
For older patients, particularly those over 75, the prospect of open-heart surgery for aortic valve replacement can be especially daunting due to the higher risks and prolonged recovery. This is where Transcatheter Aortic Valve Implantation (TAVI) has become a game-changing alternative. Instead of a large chest incision and stopping the heart, TAVI allows a new valve to be delivered via a catheter, usually inserted through a small puncture in the groin. This minimally invasive approach significantly reduces the physical trauma to the body.
The primary advantage for seniors is the dramatic reduction in recovery time and complications. While open-heart surgery requires months of rehabilitation, many TAVI patients are up and walking within a day and can return to their daily lives within weeks. This is not just about convenience; it’s about preserving muscle mass, cognitive function, and independence, which are critical for an older person’s quality of life. The procedure is typically performed while the patient is awake (under sedation), avoiding the risks associated with general anesthesia and the heart-lung machine.
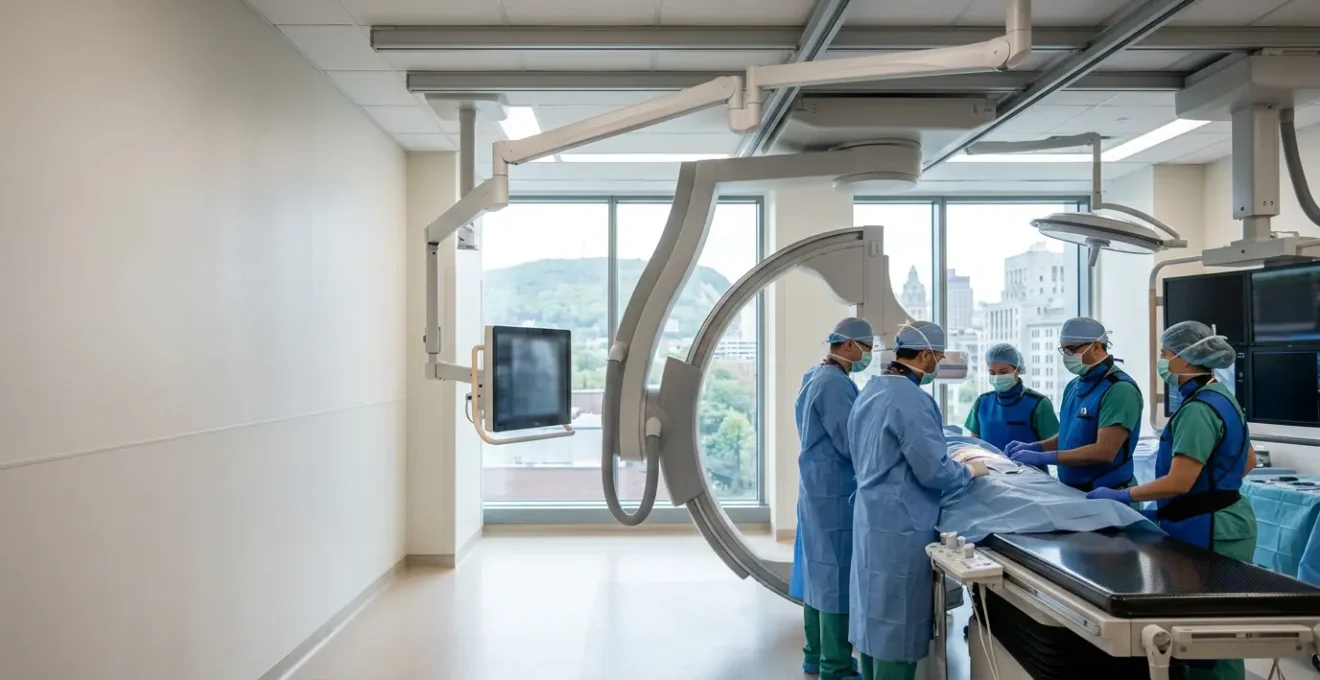
This image provides a clear visual of how the catheter-based approach allows surgeons to perform a complex valve replacement with remarkable precision and minimal invasion.
The following table, based on information from Canadian health authorities, breaks down the key differences in the recovery journey, highlighting why TAVI is often the safer and preferred path for eligible older adults.
This data, drawn from a comparative analysis by Fraser Health, clearly illustrates the benefits of the TAVI approach for older patients.
| Aspect | TAVI | Open Heart Surgery |
|---|---|---|
| Incision Type | Small puncture in groin/wrist | Large chest incision |
| Recovery Time | Days to weeks | 3-6 months |
| Hospital Stay | 1-3 days typically | 5-7 days minimum |
| Anesthesia | Usually awake/local | General anesthesia |
| Heart-Lung Machine | Not required | Required |
How to Prep for a Cardiac Catheterization to Minimize Anxiety and Complications?
The period before a cardiac catheterization can be filled with anxiety. The “what ifs” can feel overwhelming. However, you can transform this anxiety into informed confidence by taking an active role in your preparation. This is about more than just fasting; it’s a mental and logistical partnership with your healthcare team. The procedure itself is not typically painful. You will be given a local anesthetic to numb the insertion site and a mild sedative to help you relax, so you will be comfortable and often sleepy, but not under general anesthesia. Knowing this can immediately alleviate a major source of fear.
In Montreal, the healthcare system is structured to support you. At facilities like the Jewish General Hospital, patients go through a structured pre-admission clinic visit. This is your opportunity to get organized. You’ll meet with the cardiac team, review paperwork, complete pre-operative tests (like an ECG or blood work, often at your local CLSC), and, most importantly, ask questions. This systematic process is proven to reduce patient anxiety and improve outcomes because it eliminates the unknown. Don’t be shy—this is your time to seek clarity.
To make the most of this process, think of yourself as the project manager of your own health. The following checklist, based on the standard process in the Quebec system, will help you stay organized and ensure you arrive on procedure day feeling prepared and calm.
- Step 1: Obtain your medical referral from your Quebec family physician, which starts the process.
- Step 2: Diligently complete all pre-operative tests (ECG, blood work) at your designated CLSC or hospital lab.
- Step 3: Arrange for someone to drive you home. You are not permitted to drive for at least 24 hours after the procedure.
- Step 4: Pack an overnight bag with your Medicare card (carte d’assurance maladie), a complete list of your current medications, and comfortable clothing.
- Step 5: Follow fasting instructions precisely, which typically means no food or drink for 6-8 hours before your scheduled time.
- Step 6: As highlighted by the bilingual teams at Montreal’s CIUSSS de l’Ouest-de-l’Île, prepare your questions in both French and English to ensure clear communication.
The Subtle Chest Pain You Ignore That Signals a Blocked Artery
We often associate heart problems with sudden, crushing chest pain—the kind depicted in movies. While that can happen, many people experience much subtler, atypical symptoms that are easy to dismiss as indigestion, muscle strain, or anxiety. This could be a feeling of pressure, squeezing, or fullness in the chest that comes and goes. It might manifest as shortness of breath during a simple activity like climbing stairs, or unusual fatigue that doesn’t go away with rest. Pain in the jaw, neck, back, or arms can also be a sign. Ignoring these “small” signals is a significant risk, as they can be your body’s early warning system for a partially blocked artery.
The danger is that these symptoms can become your “new normal,” and you might not seek help until the blockage is severe. This is concerning because research shows that 30-40% of patients require future treatment for recurring symptoms even after an initial intervention. Early diagnosis and treatment not only prevent a major cardiac event but also lead to better long-term outcomes. Listening to your body and speaking to your doctor about any new or persistent chest-related discomfort is not an overreaction; it is essential self-care.
This reality also creates a valid concern for both patients and their families, especially when considering a rapid, same-day discharge after a procedure. As one research team noted, this anxiety is completely understandable.
Caregivers and patients often have concerns regarding same-day discharge because of the limited postprocedural telemetry monitoring.
– JACC Research Team, JACC: Cardiovascular Interventions
This is why clear discharge instructions and a confirmed follow-up plan are non-negotiable parts of a safe, rapid-recovery protocol. They provide the necessary safety net and peace of mind after you leave the hospital.
How to Restart Physical Activity After a Stent Without Fear of Relapse?
After receiving a stent, the thought of physical activity can be a double-edged sword. You know it’s crucial for your long-term health, but the fear of “overdoing it” and causing a problem can be paralyzing. The key is to reframe your mindset from fear to a structured, gradual plan. Your heart is now stronger and receiving more blood flow; activity will help it, not harm it, as long as you restart intelligently. This is about building confidence one step at a time, not jumping back into your old routine overnight.
The goal is to listen to your body and your medical team. You’ll likely be enrolled in a cardiac rehabilitation program, like the one at the world-renowned EPIC Centre at the Montreal Heart Institute. These supervised programs are the gold standard for a safe return to activity. They provide you with a personalized exercise plan and the security of having medical professionals on hand to monitor your progress and answer your questions.
Living in Montreal provides unique opportunities to stay active safely throughout the year. The key is adapting your activity to the season and your recovery stage. This image of a person walking along the Lachine Canal captures the feeling of peaceful, confident recovery that is your ultimate goal.
Here is a practical, four-season plan to help you gradually and safely reintegrate physical activity into your life in Montreal:
- Winter: Start with 10-15 minutes of daily indoor walking. Montreal’s Underground City (RÉSO) offers a vast, climate-controlled environment perfect for this.
- Spring: As the weather improves, take gentle walks in a flat, scenic area like Parc Jean-Drapeau, gradually increasing your distance each week.
- Summer: Enjoy light cycling on the beautiful, flat path along the Lachine Canal. The key is to avoid steep inclines and maintain a comfortable pace.
- Fall: Consider swimming at a local YMCA or community pool. Many offer specific times or programs tailored to individuals with cardiac conditions.
Public Hospital vs Private Clinic: Which Path Suits Your Urgency?
When facing a cardiac issue in Quebec, one of the first questions is often about navigating the healthcare system: should you go through the public system or explore private options? For urgent and therapeutic cardiac interventions like angioplasty, TAVI, or ablation, the answer is clear: the public system is not only your primary path but also a world-class one. The Montreal Heart Institute, a public institution affiliated with Université de Montréal, is the largest and one of the most respected cardiology centers in Canada, providing top-tier care entirely covered by RAMQ.
Private clinics in Quebec play a different role. They are excellent for rapid access to diagnostic tests. If your family doctor suspects an issue, you could wait weeks or months for an echocardiogram or stress test in the public system. A private clinic can often get you in within days, for an out-of-pocket fee. However, it’s crucial to understand their limitation: private clinics in Quebec are generally not equipped to perform therapeutic procedures like stenting or valve replacements. Once a problem is diagnosed privately, you will be referred back into the public system for treatment.
Therefore, the choice depends on your urgency and need. If you need a diagnosis quickly to ease your mind or to get a referral for treatment faster, the private route can be a valuable tool. For the actual intervention, the public system is your destination. The following table clarifies the distinct roles and costs associated with each path.
| Service Type | Public System (RAMQ) | Private Clinics |
|---|---|---|
| Wait Times | Variable (weeks to months for diagnostics) | Typically within days for diagnostics |
| Cost | Covered by RAMQ | $2,000-$5,000+ out-of-pocket for diagnostics |
| Diagnostic Tests | Available with referral | Available immediately |
| Therapeutic Procedures | Full range available | Limited to diagnostics only |
| Follow-up Care | Included | Additional cost |
How the Surgeon Controls the Robot: It’s Not Autonomous!
The term “robotic surgery” can be misleading. It might conjure images of a machine operating independently, which is a common source of patient anxiety. It’s essential to understand that the robot is not autonomous; it is a highly advanced tool that is 100% under the surgeon’s control at all times. Think of it as an extension of the surgeon’s hands, but with enhanced precision, stability, and dexterity. The surgeon sits at a sophisticated console, often in the same room, viewing a magnified, 3D high-definition image of the heart. Every movement of the robotic arms precisely replicates the surgeon’s hand movements.
Surgeons have learned that safe access to the part of the heart that is damaged can often be achieved without a traumatic incision.
– Dr. Allan Stewart, Minimally Invasive Heart Surgery Program
The primary benefit of this technology is that it allows surgeons to perform incredibly complex procedures through a few small incisions, typically just 2-3 inches long, instead of a large incision that requires opening the chest and splitting the breastbone. This is the essence of minimally invasive surgery. As demonstrated in leading programs like Weill Cornell’s robotic heart surgery program, this technology filters out natural hand tremors and allows for movements in tight spaces that would be impossible for a human hand alone.
So, instead of being a step removed from your care, the surgeon is more immersed than ever, with a better view and more precise tools. The robot doesn’t make decisions; it executes the surgeon’s decisions with microscopic accuracy. This combination of human expertise and technological precision is what enables faster recovery, less pain, and reduced scarring compared to traditional open-heart surgery. It is a testament to how technology serves the surgeon’s skill, rather than replacing it.
Key Takeaways
- Modern procedures like TAVI and angioplasty enable treatment and discharge in under 24 hours, avoiding the trauma of open-heart surgery.
- Your active partnership in preparing mentally, asking questions, and following a structured recovery plan is as crucial as the technology itself.
- Montreal’s public healthcare system, led by institutions like the Montreal Heart Institute, provides world-class, RAMQ-covered cardiac interventions.
Why Electrophysiology Is the Only Way to Permanently Cure Certain Arrhythmias?
For many people living with a heart rhythm disorder (arrhythmia), daily life is governed by medication. While drugs can be effective at managing symptoms like palpitations, dizziness, or fatigue, they rarely offer a permanent cure. They control the problem but don’t fix the underlying cause. Electrophysiology (EP) offers a different path: a potential cure. Arrhythmias are caused by faulty electrical signals in the heart. An EP study is like creating a detailed electrical map of your heart to pinpoint the exact location where these rogue signals originate.
Once the problematic area is identified, a procedure called catheter ablation can be performed, often in the same session. A specialized catheter is guided to the precise spot inside the heart and delivers a burst of radiofrequency energy (heat) or cryo-energy (cold) to neutralize the tiny cluster of cells causing the short-circuit. This permanently eliminates the source of the arrhythmia. It’s not about managing the problem; it’s about removing it. For many common arrhythmias, this procedure offers a definitive cure, allowing patients to stop taking medication and live without the constant worry of their heart rhythm.
The journey to a cure in Quebec follows a clear and structured path, ensuring you are guided every step of the way:
- Initial Diagnosis: Your family physician will likely order a Holter monitor test to record your heart’s electrical activity over 24-48 hours.
- Specialized Referral: Based on the results, you’ll be referred to a specialized EP lab, such as the one at the Montreal Heart Institute.
- Pre-procedural Testing: Before the procedure, you will undergo tests like an echocardiogram and blood work to ensure you are a good candidate.
- Catheter Ablation: The procedure is done under conscious sedation. It’s minimally invasive, with catheters inserted through the groin.
- Post-procedure Monitoring: You will be monitored for 4-6 hours before being discharged, often on the same day.
- Follow-up: An appointment is scheduled within a couple of weeks to assess the success of the ablation and discuss any adjustments to your medication.
By understanding these modern procedures and your role within the process, you can approach your cardiac care not with fear, but with the confidence that a faster, less invasive, and successful outcome is within reach. Your next step is to have an open conversation with your doctor to determine the best path for your specific needs.