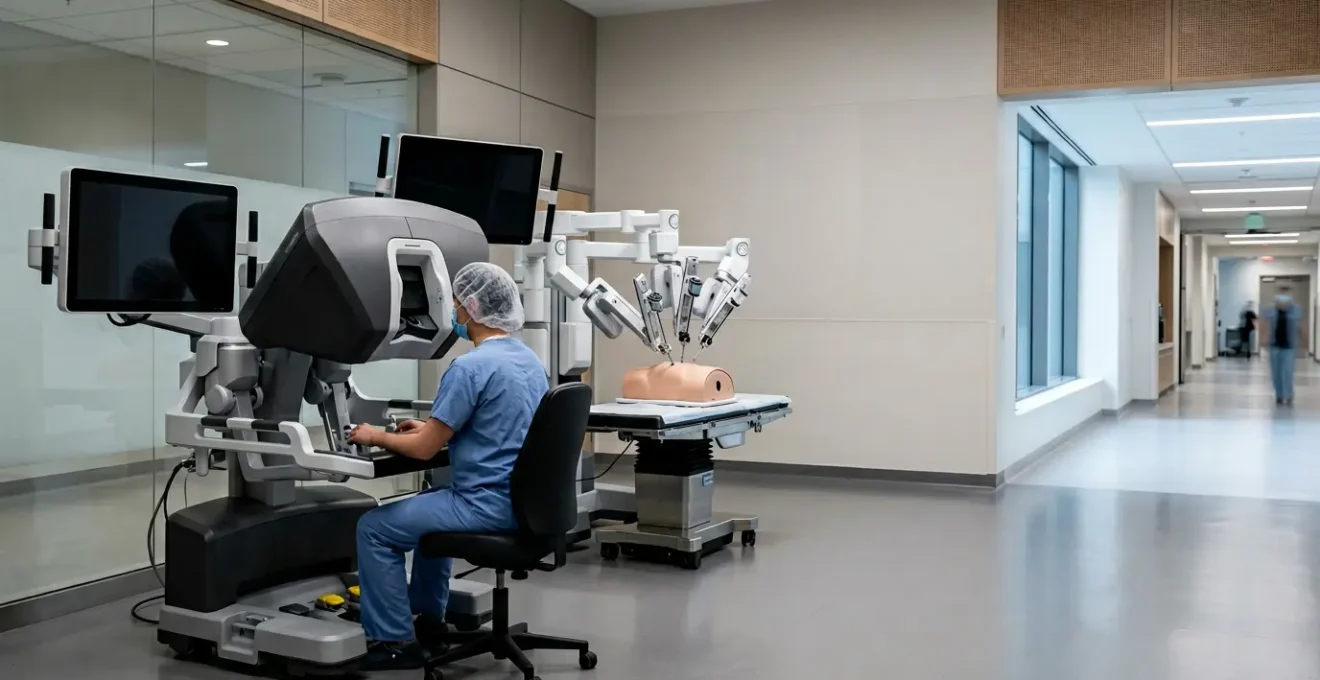
For a patient, the promise of robotic surgery isn’t the robot itself, but the surgeon’s enhanced ability to perform delicate procedures, which directly translates into a quicker, less painful recovery.
- Robotic systems provide magnified 3D vision and tremor-free instrument control, allowing for greater precision than traditional laparoscopy, especially in nerve-sparing procedures like prostatectomy.
- This enhanced precision often results in significantly reduced hospital stays and a return to normal activities weeks sooner than with open surgery.
Recommendation: Focus not on the technology, but on the surgeon’s specific experience with that technology for your particular procedure.
When you receive a diagnosis like prostate cancer, the world seems to narrow down to a single focus: choosing the best path forward. The options presented—open surgery, laparoscopy, robot-assisted surgery—can feel overwhelming. As a surgeon, I see the uncertainty in my patients’ eyes. You’ve likely heard the buzz around “robotic surgery,” often positioned as the latest and greatest, but what does that truly mean for you, the person who has to live with the outcome? The common discourse focuses on smaller scars and high-tech appeal, but these are just surface-level benefits.
The crucial conversation we need to have goes deeper. It’s not about a robot performing surgery; it’s about a highly skilled surgeon using an advanced set of tools. The fundamental question isn’t “Is the robot better?” but rather, “How does this tool in my hands allow me to achieve a better outcome for you?” This means a faster return to your life, better preservation of critical functions like continence and erectile function, and minimized postoperative pain. The key to understanding the difference lies in the mechanics of the surgery itself—the surgical ergonomics, the stability of the vision, and the articulation of the instruments.
This guide is designed to pull back the curtain. We will move beyond the marketing and explore the tangible differences from a surgeon’s perspective. We’ll demystify how these tools work, discuss what the learning curve for a surgeon really looks like, and tackle the practical questions that matter in Montréal, such as RAMQ coverage. The goal is to empower you with a clear, honest understanding so that when you make your decision, you are choosing not just a technology, but a strategy for the best possible recovery.
To provide a clear and structured overview, this article will walk you through the key questions and considerations. The following summary outlines the topics we will cover, from the fundamental control of the robot to the practical realities of recovery and cost in the Canadian healthcare system.
Summary: A Surgeon’s Perspective on Minimally Invasive Procedures
- How the Surgeon Controls the Robot: It’s Not Autonomous!
- Single-Port Surgery: How to Have a Hysterectomy with Almost No Scars?
- Does RAMQ Cover the Extra Cost of Robotic Surgery Supplies?
- How Many Robotic Surgeries Must a Doctor Do Before They Are ‘Expert’?
- Returning to Work: 2 Weeks vs 6 Weeks After Invasive Surgery?
- Angioplasty Recovery: Why Do Some Patients Feel Worse Before Feeling Better?
- Repair vs Removal: Which Meniscus Surgery Preserves Your Knee Long-Term?
- How Advanced Interventional Cardiology Reduces Hospital Stays to Less Than 24 Hours?
How the Surgeon Controls the Robot: It’s Not Autonomous!
Let’s clear up the most significant misconception right away: the robot does not perform the surgery. I do. The da Vinci system, the most common surgical robot, is a master-slave system. Think of it not as an autonomous pilot but as an incredibly sophisticated flight control system that translates my intentions with unparalleled fidelity. I sit at a console, often in the same room, with my head in a viewer that provides a magnified, 3D high-definition view of the surgical site. My hands grasp master controls, and my finger movements are translated in real-time to the robotic arms and instruments inside your body.
This setup is a revolution in surgical ergonomics. It filters out the natural tremor in a surgeon’s hands and can scale my movements; a one-centimetre move of my hand can be translated into a one-millimetre move of the instrument tip. As thoracic surgeon Dr. Jason Fitzgerald states clearly, “The da Vinci Surgical System cannot act on its own.” It is an extension of my hands and eyes. This level of control is why we can perform incredibly delicate tasks, like sparing the tiny nerves around the prostate that are crucial for function. Institutions like the McGill University Health Centre are at the forefront of this field, recently unveiling the SuPER Centre, the first and only hospital-based surgical robotics and AI research centre in Canada, to further refine these human-machine collaborations.
Single-Port Surgery: How to Have a Hysterectomy with Almost No Scars?
The evolution of minimally invasive surgery is constantly pushing towards a simple goal: achieving the same or better surgical results with less trauma to the body. Single-port surgery is a prime example of this principle. In traditional laparoscopy or even standard multi-port robotic surgery, several small incisions (ports) are made in the abdomen to introduce a camera and various instruments. While these are a vast improvement over a large open incision, they still leave multiple small scars.
Single-port robotic surgery takes this a step further. All the instruments and a high-definition camera are introduced through a single, small incision, typically hidden discreetly within the navel (belly button). Once inside, the robotic platform deploys its instruments, which have the flexibility to move and operate as if they had entered through separate ports. For a procedure like a hysterectomy (removal of the uterus), this means a major abdominal surgery can be completed leaving behind a scar that is nearly invisible once healed. This is not just about aesthetics; a single, smaller incision often means less pain, a lower risk of infection, and a faster initial recovery. Indeed, a study published in the Journal of Minimally Invasive Gynecology found that patients who underwent single-port robotic hysterectomies were highly satisfied with the scar appearance and reported low pain scores. It represents the pinnacle of the “less is more” philosophy in modern surgery.
Does RAMQ Cover the Extra Cost of Robotic Surgery Supplies?
This is a critical and entirely practical question for any patient in Québec. The short answer is yes, the surgical procedure itself, when deemed medically necessary and performed in a public hospital (like the MUHC or CHUM), is covered by the Régie de l’assurance maladie du Québec (RAMQ). You will not receive a bill for the surgeon’s time or for the use of the operating room, regardless of whether the procedure is open, laparoscopic, or robotic.
However, the conversation around cost is more nuanced. The robotic systems are expensive. Research from the Canadian Urological Association Journal highlighted that the initial purchase price can be around $2.8 million in Canada, with significant annual maintenance and per-case costs for specialized, disposable instruments. While the public system in Québec generally absorbs these operational costs for approved procedures, there can sometimes be discussions around specific high-cost disposable items. It’s important to have a transparent conversation with your surgeon’s office and the hospital’s administrative staff. They can clarify if all components of your specific robotic surgery are fully covered or if there are any exceptions. In most Canadian provinces, these costs are covered, often through a combination of public funds and hospital fundraising, ensuring patients have access to this technology without direct financial burden.
How Many Robotic Surgeries Must a Doctor Do Before They Are ‘Expert’?
This is the most important question a patient can ask, as the technology is only as good as the person controlling it. There is no single magic number, but there is a well-understood “learning curve.” Expertise is built in stages. Initially, a surgeon trains extensively on simulators. Then, they perform procedures under the supervision of an experienced proctor. Finally, they begin their own practice, with the first 20-50 cases often considered the steepest part of the learning curve where operative times decrease and efficiency improves.
However, true expertise goes beyond case numbers. It’s about consistent, excellent outcomes, low complication rates, and the ability to handle complex or unexpected situations. In major Canadian centres, this is taken very seriously. For example, the urology residency program at McGill University provides comprehensive training from the very beginning, including a robotic simulator and hands-on experience at major Montréal hospitals. This ensures the next generation of surgeons is proficient with the technology. Established programs, like the one described by the University Health Network / Sinai Health System in Toronto, explicitly state their surgeons have each completed “hundreds of complex robotic cases.” For a patient, this means you should feel comfortable asking your surgeon about their experience: “About how many of these specific procedures have you performed robotically?” An expert surgeon will be transparent and understand the importance of this question for your peace of mind.
Your Pre-Surgery Checklist: Questions for Your Surgeon
- Why is robotic surgery the recommended approach for my specific case compared to open or laparoscopic options?
- How many robotic procedures of this type have you personally performed, and what is your complication rate?
- What specific outcomes can I expect regarding my primary concerns (e.g., cancer control, urinary continence, erectile function)?
- What does the typical recovery timeline look like for your patients undergoing this procedure?
- Who will be part of the surgical team, and what is their experience with robotic surgery?
Returning to Work: 2 Weeks vs 6 Weeks After Invasive Surgery?
The speed of recovery is one of the most tangible benefits for a patient. The difference between robot-assisted surgery and traditional open surgery is not incremental; it’s a paradigm shift. An open prostatectomy, for example, requires a large incision from the navel to the pubic bone, cutting through layers of muscle. This significant trauma is the primary driver of a long, painful recovery, often involving a multi-day hospital stay and 6-8 weeks before a return to even a desk job.
Robotic surgery, by contrast, requires only a few small incisions, each about a centimetre wide. The muscles are spread apart, not cut. This dramatic reduction in tissue trauma is why recovery is so much faster. The following table provides a general comparison for a procedure like a hysterectomy, but the principles apply to many other surgeries, including prostatectomy. It clearly illustrates the difference in key recovery milestones.
| Recovery Milestone | Robotic Hysterectomy | Traditional Open Surgery |
|---|---|---|
| Hospital Stay | Same day to 1 night | 2-4 days typical |
| Return to Light Activities | 1-2 weeks | 4-6 weeks |
| Return to Desk Work | 2 weeks | 6-8 weeks |
| Full Recovery | 4-6 weeks | 8-12 weeks |
| Incision Healing | 1 week (5 small incisions ~1cm each) | 6-8 weeks (large incision) |
| Scar Visibility | Minimal, largely imperceptible | Significant visible scar |
For a patient, this data, which is consistent with sources like comparisons from gynaecology practices, translates into real-world benefits: less time in the hospital, reduced need for strong pain medication, and a quicker return to your normal life, work, and family. Being back on your feet in two weeks versus six or more is a profound difference that impacts your physical and emotional well-being.
Angioplasty Recovery: Why Do Some Patients Feel Worse Before Feeling Better?
While our main focus is on large surgical procedures, the principles of minimally invasive intervention extend to other areas, like cardiology. Angioplasty is a procedure where we use a balloon and often a stent to open a narrowed or blocked coronary artery. It’s life-saving, but some patients are surprised to feel a bit off, or even experience some chest discomfort, in the days following. This can be alarming, but it’s often a normal part of the healing process.
There are a few reasons for this. First, the area of the artery where the stent was placed is, in essence, a controlled injury. It needs time to heal, and this can cause some inflammation and local irritation, which you might perceive as a dull ache or discomfort. Second, the sudden restoration of robust blood flow to a part of the heart muscle that was “starved” for oxygen can itself be a strange sensation. The heart muscle has to readjust to this new, healthier state. Finally, the procedure itself, though minimally invasive, can cause minor bruising at the entry site (usually the wrist or groin) and a general feeling of fatigue as your body dedicates energy to healing. The key is to distinguish this from the sharp, crushing pain of a heart attack. Any severe, worsening, or concerning chest pain after a procedure requires immediate medical attention.
Repair vs Removal: Which Meniscus Surgery Preserves Your Knee Long-Term?
Moving to the world of orthopaedics, we encounter a similar philosophy of minimizing intervention to maximize long-term function. When a patient tears their meniscus—the C-shaped cartilage that acts as a shock absorber in the knee—the surgical question is often not *if* we should operate, but *what* we should do: repair it or remove the torn piece (a partial meniscectomy)?
For many years, the standard approach was to simply trim away the damaged part. It’s a technically simpler, faster procedure with a very quick initial recovery. However, we’ve learned that the meniscus plays a vital role in protecting the knee joint. Removing a piece of it, even a small one, increases the contact stress on the articular cartilage—the smooth lining at the ends of your bones. This can accelerate the development of osteoarthritis down the road. Therefore, whenever possible, the modern approach is to preserve the meniscus by repairing it. A meniscal repair involves suturing the torn edges back together. This is a more complex procedure and, importantly, the recovery is longer and more involved. It requires a period of protected weight-bearing to allow the tissue to heal. The trade-off is clear: a longer, more demanding recovery now for a much higher chance of a healthier, more functional knee in 10, 20, or 30 years. The decision depends on the type, location, and size of the tear, as well as the patient’s age and activity level, but the guiding principle is always to preserve your natural anatomy if we can.
Key Takeaways
- Robotic surgery is a tool that enhances a surgeon’s precision; it does not operate autonomously. The surgeon’s skill remains the most critical factor.
- For patients, the primary benefits are tangible: smaller incisions, less pain, reduced blood loss, and a significantly faster return to normal life compared to open surgery.
- In Québec, medically necessary robotic surgery is covered by RAMQ, but it’s always wise to confirm details with the hospital administration.
How Advanced Interventional Cardiology Reduces Hospital Stays to Less Than 24 Hours?
The ability to send a patient home the same day or the next morning after a major cardiac intervention like angioplasty is one of the great triumphs of modern medicine. It’s not one single invention, but a combination of advancements that make this possible. First is the shift from the femoral artery in the groin to the radial artery in the wrist as the preferred access point. This “transradial approach” has been a game-changer. The radial artery is smaller and more superficial, so bleeding complications are far less common and much easier to control. Patients can sit up and walk around almost immediately, instead of having to lie flat for hours to prevent bleeding from the groin.
Second, the tools we use—the guidewires, catheters, and stents—have become incredibly sophisticated, smaller, and more flexible, allowing us to navigate complex anatomy with less trauma to the blood vessels. Third, our imaging technology provides crystal-clear, real-time views of the arteries, allowing for precise stent placement. Finally, our post-procedure protocols are streamlined. By using a simple compression band on the wrist and being able to ambulate the patient quickly, we remove the need for prolonged bed rest and observation. This combination of better access, better tools, and smarter protocols means that for an uncomplicated case, the entire procedure and recovery can happen within a single day, reducing costs, lowering infection risk, and getting the patient back to the comfort of their own home.
Understanding these advanced tools and techniques is the first step. The next is to apply this knowledge to your own situation by having a detailed, confident conversation with your care team. For a decision as personal as this, having a full command of the facts is not just helpful; it is essential.